…………….
Return To Main COVID-19 Resource Page
…………….
COVID-19 Psychosis
Neuropsychiatric issues caused by COVID-19 vaccines and/or exposure to the COVID-19 virus in the wild.
Be sure to visit my COVID-19 Healing Resources page which provides a variety of treatments for COVID-19-related illnesses, including psychosis.
……………..
Nicolas Hulscher: Over 70% Of Humanity Underwent A Chemical Lobotomy Masquerading As ‘Vaccination’
……………..
Dr. Sherri Tenpenny: New Study Links mRNA Shots To Neuropsychiatric Harm
……………..
• Top Pathologist Warns mRNA ‘Vaccines’ Cause ‘Personality Changes’: ‘Pineal Gland Was Completely Destroyed’ (Frank Bergman, Slay, 04/22/25)
• Study Identifies 86 Serious Neuropsychiatric Safety Signals Linked To COVID-19 Vaccination (Nicolas Hulscher, 04/14/25)
CDC/FDA safety thresholds breached for 86 adverse events including dementia, schizophrenia, suicidal and homicidal thoughts, stroke, psychosis, depression, cognitive impairment, delusions, and more.
……………..
Dr. Bhakdi: Because Of mRNA Vaccines, The Brains Of Billions Of People Are Not Working Anymore
……………..
Dr. Malhotra: Some Vaccinated People Are Suffering From A Psychosis Called ‘The Delusion Of Benefit’
……………..
• A Horrifying Breakthrough In The WHITE FIBROUS CLOT Saga (Laura Kasner, Substack, 03/26/25)
“And now we come to maybe the most important and scariest test results of all. There is a subset of amyloid proteins called ‘prions.’ Prion diseases are a group of fatal neurodegenerative disorders caused by the accumulation of misfolded proteins in the brain. These proteins, known as prions (short for “proteinaceous infectious particles”), are resistant to conventional methods of sterilization and can cause widespread brain damage . . . In terms of prion diseases, neurovascular or neurodegenerative disorders may arise, and do so more quickly than the decades that it usually takes for these disorders to manifest. For example, neurovascular disorders such as mild cognitive impairment (MCI), brain fog, tremors, and behavioral changes may arise in younger people. And more serious neurodegenerative disorders such as Creutzfeldt-Jakob Disease, Parkinson’ disease, and Alzheimer’s-like dementia can occur in younger people as well.”
• The Conscious Clinician Compact
• Catastrophic Neurological And Psychiatric Damage From COVID-19 ‘Vaccines’ (Nicolas Hulscher, 01/05/25)
Increased risks of ischemic stroke, hemorrhagic stroke, transient ischemic attack, myelitis, myasthenia gravis, Alzheimer’s disease, cognitive impairment, depression, anxiety, and sleep disorders
• Major Study Confirms Covid ‘Vaccines’ Change People’s Personalities, Emotions (Frank Bergman, Slay News, 01/26/25)
An alarming study has provoked major new concerns about mRNA “vaccines” after researchers confirmed that Covid injections change the personalities of those who receive them . . . The peer-reviewed study, which included over 2 million participants, was published in the renowned Nature Journal . . . They explain that the “vaccines” cause “psychiatric manifestations” among the vaccinated. The study found that these psychiatric changes resulted in spikes in mental health disorders. Patients described feelings of inner turmoil, fear, dread, and depression. The study found that Covid shots triggered a 68.3% spike in depression, a 43.9% increase in anxiety disorders, and a 93.4% surge in sleep disorders…
• Are The Jabs Changing Our Personalities? (World Council for Health, 12/11/24)
Conducted by leading researchers in South Korea, this study raises alarming questions about how these ‘vaccines’ may influence emotional and psychological states.
• Are Medical Errors On the Rise Due To Cognitive Impacts Of The mRNA Vaccine? (Dr. Pierre Kory, 10/18/24)
• Association Between COVID-19 Vaccination And Development Of Alzheimer’s Disease (Dr. Peter McCullough, 06/25/2024)
• We Now Have Proof The COVID Vaccines Damage Cognition (A Midwestern Doctor, 06/20/2024)
• First Reported Case Of New-Onset Mania & Psychosis Post Bivalent mRNA COVID-19 Booster Vaccination – December 2023, from Singapore – 16 Cases In The Literature (Dr. William Makis, 02/02/24)
……………..
Dr. Peter McCullough Interviews Lynnette Milakovich (COVID-19 Vaccine & Brain Damage)
My Story: The COVID-19 Vaccine and Brain Damage
……………..
Psychosis, Panic Attacks, Hallucinations: Bizarre Psychiatric Cases Among The COVID Vaccinated
By Marina Zhang
The Epoch Times
October 3, 2023
Download a pdf copy of this article
Dr. Patrick William Slater is a 60-year-old neurotologist. A few years ago, he had a full-time medical practice in Austin and enjoyed hunting and fishing in the mountains during his downtime.
Then, in October 2021, Dr. Slater came down with cerebellar ataxia, a disease affecting movement. He couldn’t eat or go to the bathroom without help.
While his ataxia could be managed using drugs, it wasn’t always effective against his biggest complaint: unprecedented panic attacks.
Almost every night, Dr. Slater would experience panic attacks that left him in “abject terror.” He thought about killing himself many times, he told The Epoch Times.
No one could provide a satisfactory answer about why he had developed these symptoms. Nothing abnormal showed up on his laboratory reports, and his neurologists and psychiatrists dismissed his symptoms as anxiety.
But Dr. Slater is convinced that the COVID-19 mRNA vaccines are the culprit.
Dr. Slater was suspicious when the symptoms first appeared within about two weeks of getting the second dose of the COVID shot. The second — and worse — wave of career-ending symptoms had coincided with his third shot.
After taking the booster, “there was no question in my mind,” Dr. Slater said.
Increase in Unusual Psychiatric Illness
Beginning in late 2020 with the COVID vaccine rollout, some doctors have seen an increase in unusual psychiatric illnesses.
Psychiatrist Dr. Amanda McDonald noticed a wave of psychiatric destabilization among her stable patients. They experienced flare-ups, often manifesting with worsened or new psychiatric symptoms.
“I couldn’t figure out why,” Dr. McDonald told The Epoch Times. “My patients typically stay stable.” But many stable patients were suddenly arriving at her office with insomnia, depression, and anxiety “without any sort of rhyme or reason.”
She increased some patients’ medication doses or added new drugs to their regimen, but it had little effect.
A recurring pattern Dr. McDonald sees is atypical panic attacks, which can feel like having a heart attack. Brought on with no apparent trigger, symptoms typically escalate as the evening progresses and climax at night. A typical panic attack can occur anytime throughout the day but often has triggers, and it is easy to treat if patients can avoid these triggers.
After spending over a year following her patients, Dr. McDonald realized that COVID-19 vaccines may be linked to their psychiatric illnesses.
“I already had an existing patient population when the pandemic hit that I knew very well. What I saw was manifestations in that patient population,” Dr. McDonald added.
Dr. Diane Counce, neurologist and neuroradiologist, observed an increase in severe anxiety and worsened mood.
“People also talk about how their personality has changed,” she told The Epoch Times. In cases where a family member has brought in a patient, “[The family] will say, ‘they’re just different.'”
Nurse practitioner Scott Marsland, who has treated hundreds of long-COVID and vaccine-injured patients at the Leading Edge Clinic, added that debilitating anxiety, depression, and insomnia are among the most common symptoms he has seen. However, some patients have also developed hallucinations and suicidality.
The Evidence
Unlike myocarditis, no conclusive proof exists that COVID-19 vaccinations cause psychiatric illness. A multitude of studies, however, have linked COVID-19 vaccines with psychiatric symptoms, including depression, anxiety, panic attacks, psychosis, and suicidality.
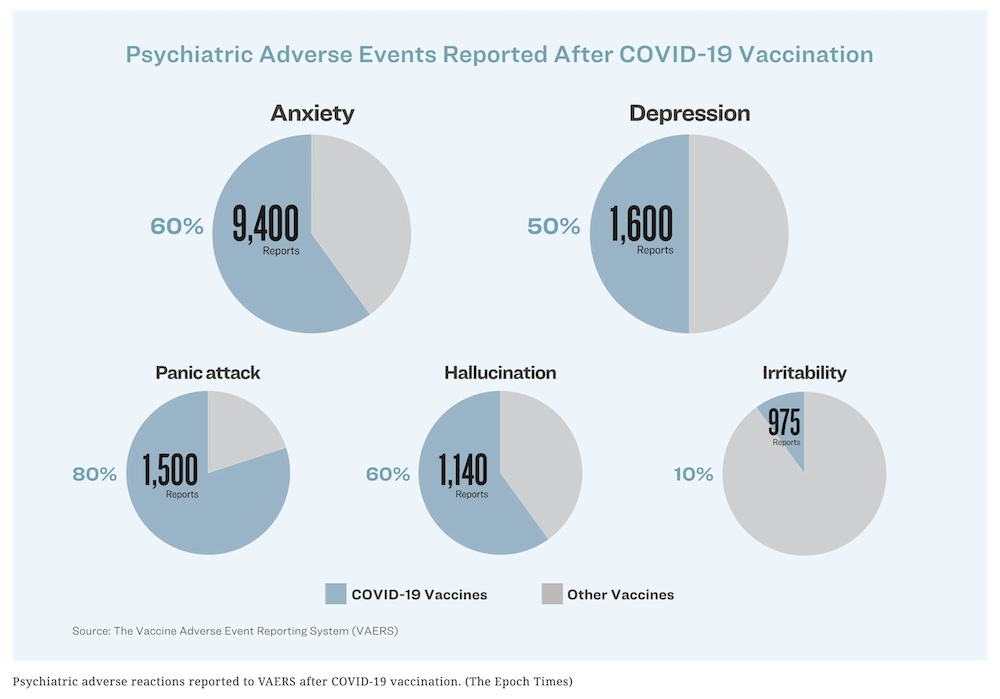
The Vaccine Adverse Event Reporting System (VAERS) is a self-reporting database co-managed by the U.S. Centers for Disease Control and Prevention (CDC) and the U.S. Food and Drug Administration (FDA), used to surveil for early warning signs of potential adverse reactions. VAERS has documented over 9,400 and 1,600 cases of anxiety and depression, respectively, in relation to the COVID-19 vaccines. The vaccines comprise, respectively, over 60 percent and up to 50 percent of all anxiety and depression reports on VAERS.
Other less common adverse reactions include 1,500 reports of panic attacks (over 80 percent of VAERS reports), over 1,100 cases of hallucinations (over 65 percent), and 975 cases of irritability (10 percent).
Some researchers argue that the rare and fatal cases reported on VAERS may be a sign the system is being abused. In contrast, others believe they suggest a potential link to the vaccine and are worth investigating.
Psychosis
Psychosis includes both hallucinations and paranoia. Acute episodes after taking the shots have been reported in case studies.
In Brazil, a previously healthy woman in her late 30s developed refractory psychosis within 24 hours of getting the mRNA COVID-19 vaccine. She was aggressive, had disorganized thoughts, and believed she was being persecuted in the hospital.
Doctors treated her with antipsychotics and mood stabilizers, but four months of hospitalization later, only her behavior had improved. Her psychosis remained.
In Taiwan, a 15-year-old boy was sent to the hospital with agitation and uncontrollable limb stretching and screaming two days after his second Pfizer shot.
He exhibited bizarre behaviors in the hospital, including sitting up and lying down frequently with mannerisms like praying in the bed. He was prescribed antipsychotics, but the behavior persisted for over a month after discharge.
Doctors then put him on a steroid regimen. Steroids are anti-inflammatory and can help calm an overactive immune system. The boy’s symptoms improved.
In India, a 17-year-old girl who received an inactive COVID-19 vaccine developed psychosis within 48 hours. She became restless and suspicious, talked to herself, and had insomnia for a month.
She had no neurological abnormalities, and all her lab tests came back normal, including a COVID-19 test. Two weeks after being given psychoactive drugs, her symptoms resolved.
Symptoms onset shortly after vaccination, exclusion of other likely causes, and absence of genetic predisposition “indicate the psychiatric adverse event may be related to the vaccine,” researchers from All India Institute of Medical Sciences and District Hospital wrote in the case report.
Cases of psychosis lasting several days, weeks, and months have also been reported in the literature.
Suicides and Suicidality
According to React19, a nonprofit advocacy group supporting people with postvaccine symptoms, suicide is a present risk for people with vaccine injuries. However, often, it is hard to determine whether people become suicidal due to their injuries becoming too unbearable or due to a primarily physiological reaction to the vaccine.
The CDC’s review of deaths reported after Pfizer vaccines found 14 deaths among vaccinated teenagers, two of whom died by suicide, with reasons unknown.
A study on 250 dental staff in Pakistan found that nearly 12 percent reported suicidal thoughts for a few days after vaccination. Around 1 percent had thoughts of suicide every day.
Individual case studies identified a Turkish man in his late 50s with no prior mental illness who arrived at the emergency department due to an attempted suicide within three days after taking a second shot. He was irritable, insomniac, and talking to himself.
A Japanese man’s case was vividly detailed by doctors from Wakayama Medical University (pdf).
He experienced fatigue after the first booster shot and, upon his fourth shot, developed a mild headache and a floating sensation.
Four days after vaccination, however, he became highly talkative with grandiose delusions, “saying that he had won 2 billion yen in horse racing. He also presented with emotional instability, such as crying when saying ‘Everyone would be happy.'”
The neurologist he saw found no neurological disorders, such as possible encephalitis, nor signs of infection. Over a week after vaccination, he jumped from the second floor of his house and was returned to the hospital by ambulance.
Suicide cases have been rising in the United States since the pandemic. In 2020, the CDC reported up to 46,000 suicides (pdf). This number increased to over 48,000 in 2021, and in 2022, nearly 50,000 people died by suicide. While pandemic restrictions like lockdowns and long COVID have been linked with suicides, no studies currently link increasing suicide rates with the COVID-19 vaccine.
Overlap With Cognitive Impairments
Psychiatric symptoms can also overlap with cognitive impairments like reduced memory. Dementia, for example, can manifest symptoms like depression.
Dr. McDonald treated a vaccinated patient who developed dementia-like depression. The patient, despite being in her 90s, was highly independent and lived by herself. After getting the booster, she was diagnosed with dementia and placed in a nursing home.
Taking ivermectin reversed her symptoms.
Neurologists like Dr. Suzanne Gazda, however, are concerned about untreated cases. “There are so many people that don’t even realize that they’re injured.”
Dr. Gazda has an integrative practice that treats thousands of patients with neurodegenerative diseases, and many report symptoms of cognitive decline with psychiatric symptoms.
Dr. Counce also has several vaccinated patients who developed brain atrophy. One patient had hippocampal atrophy with symptoms of memory loss and personality changes.
Dr. Counce reasoned that if the hippocampus, which serves as the brain’s memory center, atrophies, the adjacent limbic system, which processes emotions, may be similarly affected.
Possible Causes
But how exactly can vaccines lead to a person’s change of mental status and personality?
According to doctors who treat both postvaccine and post-COVID conditions, the two syndromes are quite similar in their symptoms.
Both the COVID-19 virus and the vaccines expose patients to the viral spike protein, which could cause inflammation. Depression is the disease best known for correlating with inflammation, though bipolar disorder, schizophrenia, and anxiety are also linked.
mRNA technology has long been studied, and pre-2020 research clearly shows that mRNA vaccines are highly inflammatory, holistic psychiatrist Dr. Aruna Tummala told The Epoch Times.
Dr. McDonald has found that anti-inflammatory drugs and therapeutics, such as ivermectin, hydroxychloroquine, and hyperbaric oxygen therapy, often help patients stabilize their moods.
She prescribed ivermectin for her psychiatric patients who were destabilized after taking the vaccines and saw significant improvement.
As a doctor who treated hundreds of vaccine-injured and long-COVID patients, one day, she herself developed long COVID after infection. She woke up with unexplainable negative thoughts. “I put myself in a hyperbaric machine,” she recalled, and 10 minutes after, “my mood symptoms had disappeared.”
Blood clotting, a common harm caused by spike protein, reduces the oxygenation of tissues and renders them unable to function at optimum levels, forcing them to age.
Blood clotting in the brain can cause cognitive impairments and symptoms of anxiety, depression, and psychosis as neurons become stressed and damaged.
Dr. Counce had one patient who reported anxiety, erectile dysfunction, and visual impairment. Upon taking medication for his erectile dysfunction (vasodilator drugs that increase blood volume), his visual problems improved. Realizing that the patient had microclotting, Dr. Counce put him on aspirin and nattokinase and saw positive effects.
Spike protein can also directly harm the brain, possibly leading to a disturbance in brain activity and psychiatric problems.
It can also infiltrate immune cells, causing them to release histamine. Histamine can enter the brain and inflame and irritate the nerves.
Neuroinflammation has been linked to suicidality, and a type of anti-histamine medication has also been linked to reduced suicide.
Mr. Marsland has a postvaccine patient who only had physical symptoms. One day, the patient suddenly became suicidal.
After a painstaking conversation, Mr. Marsland figured out that the only change the patient made was switching from black tea to pu-erh tea.
“Pu-erh has incredibly high histamine content,” Mr. Marsland explained. “So he stopped drinking it, and guess what, within two days, he was back to baseline.”
Infections with certain viruses have also been linked with mental impairment. The COVID-19 virus and its spike protein have been shown to reactivate ancient viral genes in our bodies.
These genes are called human endogenous retroviruses, also known as HERVs, said Dr. Adonis Sfera, a psychiatrist at Patton State Hospital. HERVs are a family of viruses within the human genome.
Activation of HERVs is linked to psychiatric symptoms like schizophrenia.
Spike protein can also reactivate the Epstein-Barr virus (EBV). EBV infections are similarly linked with psychosis.
COVID-19 vaccines have also been shown to damage the gut microbiome, possibly leading to psychiatric symptoms since many of our neurotransmitters are produced in the gut.
The Bigger Problem
While patients with vaccine-related psychiatric illnesses can often be treated, what’s concerning is that some vaccine-injured patients are diagnosed as mentally ill even though they aren’t.
Many patients develop physiological symptoms after vaccination. When they went to doctors for help, some were not taken seriously and dismissed as being anxious or stressed, said Mr. Marsland.
Nicole Sclafani, a former charge nurse at an emergency department, developed visual problems and chronic muscle pains three months after taking her primary vaccine doses. Her symptoms were exacerbated after she contracted COVID-19, and she said that neurologists, rheumatologists, and even her gastroenterologist prescribed her antidepressants.
“I’ve even had a neurologist say, ‘I would be doing you a disservice if I didn’t tell you that all of your symptoms are from stress,'” Ms. Sclafani told The Epoch Times.
When she first saw doctors, she told them she considered vaccine reaction to be a possible cause. She has since given up telling them this.
“Almost every doctor, if I said it was the vaccine, you could see their face … I was a nurse, I know that look,” Ms. Sclafani said.
Vaccine injuries manifest as a constellation of uncommon symptoms, and some doctors are reluctant to recognize these as related to the vaccine. So rather than looking at the underlying pathology, doctors often write off their patients’ symptoms as psychosomatic. Some are given a functional neurological disorder diagnosis and prescribed psychiatric medications instead.
Functional neurological disorder is poorly defined, according to psychiatrist Dr. Cristian Ciora, who is trained in psychoanalysis. It refers to a condition in which the mind finds a solution to psychological difficulties by creating physical symptoms.
“It shouldn’t be a wastebasket diagnosis. You have to have some kind of proof that the mind produces those things, and that’s not easy,” he said.
Moreover, the vaccine-injured are more likely to experience side effects and paradoxical reactions from psychoactive medications, Dr. Ciora has noticed from talking to patients.
Studies show the lipid nanoparticles carried in the mRNA vaccines interact with psychotropic drugs. Some drugs may persist longer in the patient, and a normal dose may become toxic.
Some psychiatric medications like lithium and fluvoxamine have anti-inflammatory properties and may be neuroprotective. However, many are potentially harmful. This includes the most widely prescribed antidepressant, escitalopram, with one study showing that it can change the architecture of a previously functional brain.
Paranoia in a Paranoia-Inducing World
Some vaccine-injured patients become anxious before seeing doctors, and some find it difficult to trust them.
After more and more doctors prescribed her antidepressants, Ms. Sclafani became paranoid about their medical decisions.
Despite her low sodium levels, doctors prescribed her selective serotonin reuptake inhibitors (SSRIs) or serotonin and norepinephrine reuptake inhibitors (SNRIs) — which could be dangerous as they lower sodium levels. She told the doctors about her medical condition, but they did not seem to listen.
“I am afraid that the doctor didn’t care enough, listen enough, pay attention enough,” Ms. Sclafani said. “The example about the sodium, if you were paying attention, you never would have prescribed [those drugs]. So that’s where I leave the office. I go fill the prescription, and then I never take the medication. From a psychiatric point of view, that might constitute paranoia, but I think it’s validated.”
Vaccine-injured people, especially those who took the vaccine out of goodwill, may experience both a breakdown of their worldview and of themselves, said Dr. Ciora.
He uses the iconic scene from the movie “The Matrix” as an analogy.
Neo, the main character, takes a red pill and discovers that he has been living in a machine-generated reality for his entire life. He cannot accept this reality, and vomits in disbelief.
For the vaccine-injured, the people they once trusted — health officials and government leaders — now dismiss their lived realities.
“If everyone says you’re wrong while telling you things you know to be false, you don’t know what to trust,” Dr. Ciora said.
And, you don’t know what’s reality and what’s not, he added.
……………..
Acute Psychosis After COVID-19 Vaccination
Alarming Manuscripts Report Acute Neuropsychiatric Symptoms
By Dr. Peter McCullough
January 30, 2023
Unvaccinated patients have mentioned half-jokingly that COVID-19 vaccination in friends and family makes some of them “crazy.” While I have always brushed this off as fear driven vaccine ideology taking over common sense in some zealots, the building literature on neuropsychiatric symptoms is alarming. There are now ~10 papers describing headache, fever, and a range of acute neuropsychiatric symptoms after both mRNA and adenoviral COVID-19 vaccination. The strong bias among editors and publishers has kept countless papers out of the mainstream medical media, hence one has to look far and wide to find information on the topic of vaccine safety. Borovina et al, from Croatia described three cases of acute headache followed by psychosis.
All three patients required hospitalization with exhaustive diagnostic testing and medical treatment. One of the cases progressed to attempted suicide with a knife stabbing to the abdomen requiring emergency abdominal surgery. As a doctor I am disturbed by medical evidence demonstrating gene coded SARS-CoV-2 Wuhan Institute of Virology Spike protein in the human brain after vaccination. I wonder how many subtle changes go clinically unrecognized. Even if a small number are affect, the massive numbers who came forward make any “rare” complication a common issue to face in clinical practice.
In conclusion, we should not downplay or attempt to normalize neuropsychiatric symptoms after COVID-19 shots. Every case should be taken seriously. Suicides after December 10, 2020 should be investigated and the brand, doses, and dates of vaccination should be recorded by healthcare personnel and noted by family members.
……………..
Depression, Psychosis & Suicide Ideation
Dr. William Makis
August 19, 2023
“The Dark side of Pfizer & Moderna COVID-19 mRNA Vaccine effects on the BRAIN. I review 9 studies on Suicidality, 12 on Psychosis, 5 on Depression!”
PDF Version of Article
Original Article (requires subscription)
……………..
Over 100,000 Psychiatric Disorders Like Hallucination & Suicide Reported After COVID Vaccination
GreatGameIndia
December 1, 2021
Hallucinations, anxiety, sleep disorders, psychosis, and suicide are some of the several psychiatric disorders following COVID shots that were reported in more than 100,000 cases.
Acute Psychosis
As reported by GreatGameIndia earlier, a shocking case of vaccine adverse event was documented where a healthy 20 year old young woman suffered acute psychosis one week after receiving Pfizer COVID vaccine.
Her blood pressure was high and she still had a racing heart, so she was admitted to the hospital. The following day, she took off her clothes in the hospital and proceeded to defecate on the floor.
While researchers describe this as “first instance of anti-NMDAR encephalitis after receiving the Pfizer-BioNTech COVID-19 vaccine,” other reports of a sudden onset of psychosis after COVID vaccination have already been reported and documented.
Communicating with the Dead
A report published in Psychiatry Research in October describes a 31-year-old single Hispanic office manager who was rushed by police to an emergency room for “erratic and bizarre behavior”.
He was anxious, guarded and claiming to be a “clairvoyant” able to communicate with the dead, hearing “people drumming outside his house” and a constant voice of a colleague he believed to be his lover, but had no romantic relationship with.
Symptoms began a month earlier as he received his first dose of mRNA based COVID-19 vaccine, according to reports from doctors at Stony Brook University and Northport Veteran Administration Medical Center in New York City.
They gradually got worse until he was admitted to the neurology department at the hospital. The next day, he walked around the unit talking to himself, saying that EEG machine was communicating with him.
He was given antipsychotic medication and his hallucinations subsided two days later. He was released on medication five days later, a week later he recovered and returned to work.
Nihilistic Delusions
Another case describes a 42-year-old man suffering from a horrific fraud that initiated on the day he got his Pfizer mRNA vaccine and a 57-year-healthy man who was admitted to the psychiatric emergency medical unit after he attempted suicide after three days of taking the vaccine.
Symptoms of dementia began the evening he received the vaccine, when he became irritable, sleepless, and began talking to himself and developed “nihilistic delusions”.
Living in Pure Hell
This phenomenon has also been reported in children. A report addressed to the U.S. Government’s Vaccine Adverse Event Reporting System (VAERS) describes a 13-year-old girl who developed “extremely elevated anxiety, nonstop worries and fears, irrational thoughts, OCD thoughts and behaviors” that materialized after Pfizer injection in June.
Another child, who had a tingling sensation in his limbs and sharp electric-like-jolts of pain in his brain, would lay under the blanket for hours, terrified of the world, having difficulty sleeping, tics, anger outbursts and often stared blankly.
He was later diagnosed with “autoimmune encephalitis” and could not take care of himself and now needed a full-time caregiver.
Other VAERS reports explain that the lives of young people are being ruined. One woman reported that her 28-year-old son was forced to get the vaccine by his employer and was hospitalized for two days after receiving his first dose of Pfizer.
After the shot he fell into “such a severe state of psychosis that he tried to jump out of my vehicle going 40 miles an hour.” She reported that they have been living in ““pure hell” since receiving the vaccine.
Psychosis ending in Suicide
A 48-year-old Tennessee woman who took the Pfizer vaccine said she had a psychotic episode on the same day.
“I literally thought I was going to drive myself and my nephew to Heaven… I left the house without a phone and drove all the way to where my vehicle ran out of gas. I was apprehended by the highway patrol and taken to the local hospital”.
The woman said she refused to eat, drink or sleep because of the paranoia of the thoughts that people were trying to kill her and had to stay in the hospital for two days. She was put to sleep under medication and woke up to be cured.
121,559 Psychiatric Disorders
World Health Organization’s global drug database of adverse drug events, VigiBase, lists 121,559 cases of psychiatric disorders following COVID vaccine administration. These include:
• 29,661 individuals reporting insomnia
• 18,377 reports of anxiety
• 13,904 reports of a “confusional state”
• 11,447 reports of sleep disorders
• 6,234 reports of “nervousness”
• 5,202 people reporting “disorientation”
• 4,463 reports of “acute stress disorder”
• 3,682 people who experienced “restlessness”
• 3,430 people reporting hallucinations
• 3,405 reports of depression
• 3,301 reports of “depressed mood”
• 2,814 “panic attacks”
• 2,444 people who experienced “poor quality sleep”
• 1,883 experiences of “delirium”
• 1,864 people reporting “agitation”
• 1,752 reports of nightmares
• 1,507 people who reported having “abnormal dreams”
• 606 eating disorders
• 365 cases of “psychotic disorder” or “acute psychosis” or “psychotic behavior”
• 226 instances of tic disorder
Some of the rare reports on VigiBase include 213 reports of near-death experience after vaccination, 57 suicides, and 25 cases of “exploding head syndrome” – a condition in which people hear loud noises such as explosions, gunshots or cymbals clanging as though it is right next to them, often making them as though they were sleepy or on the cusp of waking up; but it is not real.
British Yellow Card adverse event reporting data alone includes 26,916 psychiatric disorders following COVID vaccination.
Cytokine Storm Can trigger Psychosis
“The virus that causes COVID (SARS-CoV-2) is known to trigger a powerful immune response, which includes the release of large amounts of proinflammatory cytokines,” noted New York researchers in their case report.
“It has been hypothesized that a COVID-19 triggered cytokine storm may increase the risk of psychosis.” They cited 42 reported cases of psychotic behavior following COVID infection. Similarly, schizophrenia has been linked to inflammation in the recent research. Vaccination, designed to trigger an inflammatory reaction, can also go wrong.
A 2018 study of 41 people of college age looking at some inflammatory markers before and after taking the vaccination found that 41 seniors in college after receiving influenza vaccine found that those with high levels of serum interleukin-6 (IL-6) after vaccination were prone to showing signs of severe depressive symptoms.
In a 2017 pilot study, researchers at Yale University School of Medicine and the Pennsylvania State University College of Medicine reviewed vaccine records and found that children diagnosed with neuropsychiatric anorexia nervosa, obsessive compulsive disorder (OCD) and tic nervous system, may have have been vaccinated more recently than controlled children.
Vaccine induced Neurodegenerative Diseases
Meanwhile, nerve disorder Guillain Barre Syndrome has been officially added as a side effect for the AstraZeneca COVID vaccine branded as Covishield in India.
As reported by GreatGameIndia earlier, a shocking study revealed the terrifying dangers of mRNA COVID-19 vaccines inducing prion-based disease causing your brain to degenerate progressively.
The mRNA vaccine induced prions may cause neurodegenerative diseases because long-term memories are maintained by prion-like proteins.
The study concluded that mRNA based vaccine may also cause ALS, front temporal lobar degeneration, Alzheimer’s disease and other neurological degenerative diseases in the vaccine recipients.
……………..
Do The Covid Vaccines Impair Your Ability To Think?
Examining Some Of The Common Neurological Injuries Caused By Vaccination
A Midwestern Doctor
July 20, 2023
Excerpt:
One of the most common types of injuries from pharmaceuticals are neurological injuries which both impair cognitive function and create psychiatric symptoms. This places patients in a difficult situation of being gaslighted by the medical system. This is because their doctors assume the psychiatric symptoms the patients are experiencing are the cause of their illness rather than a symptom of it, leading to the patient being told the illness is all in their head and continually referred for psychiatric help. One of the best examples with this occurred as a result of the abnormal heart rhythms (e.g., rapid anxiety provoking palpitations) caused by the vaccine damaging the heart which were consistently diagnosed as being a result of anxiety, even when a subsequent workup I requested showed heart damage was present.
As I began seeing more and more signs of cognitive impairment following vaccination, I realized that what I observed mirrored what I previously seen with chronic inflammatory conditions such as mold toxicity, HPV vaccine injuries, and lyme disease. Some of the examples included:
• Many people reported having a “COVID” brain where it was just harder for them to think and remember things. I sometimes saw this after more severe cases of COVID, more frequently after vaccination, and repeatedly in patients who per their timeline clearly developed it from the vaccine but believed it had come from COVID.
• These issues tended to be more likely to affect older adults, but younger ones were more likely to notice (and complain) about them. In the case of older adults, I typically learned about them from someone else who had observed the cognitive decline rather than directly from the individual.
• I saw cases of vaccine injured individuals who had trouble remembering or recalling the word they knew expressed what they were trying to communicate (this is also a common mold toxicity symptom).
• I had friends and patients who told me their brain just didn’t work the same since they’d received the vaccine. As an example, a few colleagues told me they started losing the ability to remember basic things they needed to practice medicine (e.g., medication dosages for prescriptions). They shared that they were very worried they would need to take an early retirement and that they thought it came from the vaccine but there was no one they could talk to about it (which understandably created a lot of doubt and anxiety).
• I saw cases of coworkers demonstrating noticeable (and permanent) cognitive impairment after I’d assumed they’d received the vaccine. Their impairment was never mentioned or addressed (rather the physician kept on working, did not perform as well, and in some cases retired).
• I met significantly injured vaccine injured patients who told me one of the primary symptoms was a loss of cognitive functioning they had taken for granted throughout their life. In many cases following treatment of their vaccine injury, their cognition also improved.
• One of my friends (a very smart immunologist) developed complications from the first two vaccines and based on their symptoms was able to describe exactly which parts of their immune systems were becoming dysregulated. Against my advice, they took a booster and reported they suffered a significant cognitive impairment never experienced before in their lifetime. I feel this case was important to share as it illustrates how an exacerbation of a vaccine injury can also cause an exacerbation of cognitive symptoms.
……………..
Long COVID-Induced Neuropsychiatric Risks Can Last Beyond 2 Years; 1 Remedy To Protect From Or Reverse The Situation
No Previous Study Of COVID-19 Cases Has Achieved Such Effective Concurrent Control
By Dr. Yuhong Dong & Mercura Wang
The Epoch Times
September 12, 2022
In this article, we examine the longest and largest study on COVID-19 neurological sequelae and the fundamental cause of COVID-19 injury to our nervous system. Targeting the root cause, we may potentially reverse the situation and potentially live longer.
The medical journal Lancet Psychiatry recently published a large-scale study of the neuropsychiatric sequelae of the COVID-19 infection.
A sequelae is a pathological condition resulting from a disease, or a secondary consequence or result of that disease.
This study is an analysis of retrospective cohort studies by seven scientists from Cambridge University and Oxford University in the United Kingdom, led by professor Paul Harrison, a psychiatrist at Oxford University.
The studies spanned four continents (with data collected from the United States, Australia, the UK, Spain, Bulgaria, India, Malaysia, and Taiwan) and 62 medical institutions. The studies were conducted over a period of two years and three months, from January 2020 to April 2022.
From the electronic medical records of approximately 89 million patients, the researchers identified more than 1.28 million cases of COVID-19 infection and matched them to a cohort of non-COVID patients who were suffering from other respiratory infections. That is, they matched exactly to the experimental group in terms of age, gender, occupation, risk factors for diseases, and vaccination status, during the same time period. There were more than 1.2 million patients each in the experimental and control groups.
No previous study of COVID-19 cases has achieved such a large and well-matched concurrent control group.
The analysis evaluated two-year time-varying hazard ratios for 14 neurological and psychiatric sequelae of COVID-19 infection. These disorders included:
• Brain fog, dementia, Parkinson’s disease, and insomnia
• Anxiety disorders, mood disorders, and psychosis
• Epilepsy, encephalitis, intracranial hemorrhage, and ischemic stroke
• Guillain-Barré syndrome, neurological root and plexus disorders, and neuromuscular joint and muscle disorders
Of the 1,284,437 patients with the COVID-19 infection, their mean age was 42.5 years, ranging from children to the elderly.
Higher Mortality Risk in COVID Group Than Control Group
This analysis has provided us with very valuable information.
First, at six months after diagnosis, most of the 14 neurological and psychiatric disorders still had a significantly higher risk of morbidity among COVID patients than non-COVID patients.
Second, even at the end of the two-year follow-up period, the risk of cognitive deficits (i.e., brain fog), dementia, psychosis, Guillain-Barré syndrome, and epilepsy remained elevated, with far-reaching health consequences.
Let’s use dementia, a typical symptom, as an example to explain the situation.
By comparing the cumulative incidence of dementia in the COVID-infected group and the group of patients with other respiratory infections (i.e., the control group), it was found that at six months of diagnosis, the risk of dementia was significantly higher in the first group than in the control group.
This risk remained higher in the first group than that of the control group at the end of the two-year follow-up period.
Another typical symptom is brain fog, whose hazard ratio remained higher than that of the control group at six months after diagnosis, as well as after two years.
The risk of common mental abnormalities such as mood disorders and anxiety disorders recovered after one to two months.
The risk of psychosis, neuromuscular disorders, dementia, and brain fog is significantly higher in adults older than 65 years. The proportion of elderly patients who developed any of these neurological and psychiatric sequelae over two years was as high as approximately 32 percent, and the proportion of these elderly patients who developed these neuro-psycho sequelae who died during the two-year follow-up was as high as 34.1 percent.
Of particular note, those older adults diagnosed with dementia, brain fog, or epilepsy had mortality rates of 71 percent, 61 percent, and 83 percent, respectively, over the two-year follow-up period.
It’s obvious that the above information is a sign of serious illness. In other words, the occurrence of dementia and brain fog in the follow-up of these elderly patients portends a rather unfavorable prognosis for them.
The Severity of Sequelae Varies Among Different Variants
In addition, the researchers had also analyzed information of different COVID-19 variants, including Alpha, Delta, and Omicron during the long follow-up period. This type of unique data has rarely been provided by other studies.
The Delta variant has significantly increased risks for majorities of both the incidence of neurological or psychological sequelae such as ischemic stroke, epilepsy, brain fog, insomnia, and anxiety, and patient mortality.
The Alpha variant has caused no change in either the incidence or mortality.
The incidence of several neuropsychiatric sequelae was significantly increased after Omicron variant infection, such as dementia, mood disorders, and neurogenic disorders. However, there was no increase in patient mortality.
Why Do Neuropsychiatric Impairments Persist for 2 Years After Infection?
From the above information, we can see that even two years after COVID-19 infection, the incidence of some neuropsychiatric sequelae was still persistently higher than that of the control group.
This is an indication that the SARS-CoV-2 virus is indeed different from other viruses as, on the neuropsychiatric aspect, once a patient is injured, it isn’t easy for him or her to recover.
Research in this area is proliferating and has been a topic of interest to researchers for a long time.
According to two articles published separately this year, in the journals Science in January and Nature in July, the SARS-CoV-2 virus can directly or indirectly cause nerve cell damage. There are at least seven mechanisms through which the virus may affect the body’s nerve cells long after acute infection.
1. It directly causes apoptosis of neuronal progenitor cells.
2. It attacks the blood vessels of the brain, causing ischemia and hypoxia.
Endothelial diseases can lead to damage or fragility of the cerebral blood vessels, thrombotic events, or leaks.
3. It causes autoimmune attacks. Autoimmunity not only attacks the virus, but may also attack the components of one’s own neurons, including the outer protective layer of nerves (myelin), which has a similar function as the insulation skin of electrical wires. Once myelin is destroyed, our nerves won’t be able to transmit neuronal signals as fast as we could. That’s one of the reasons that we think, respond, and move more slowly.
4. It causes the nervous system inflammation that induces injuries to our normal nerve cells.
5. It causes mitochondrial damage to nerve cells. The mitochondria are a cell’s power plant. Once the mitochondria in nerve cells are damaged, the nerves lose their power supply and won’t be able to function properly.
6. It impairs nerve cell lipid metabolism. Lipids account for 60 percent of the brain. Lipid disorders directly link to the dysfunction of the neuronal system.
7. It inhibits autophagic activity. Autophagy is a mechanism by which nerve cells renew themselves and remove waste. The autophagy process is like our internal waste recycling system. The inhibitory effects on autophagic process will cause more garbage to accumulate without an efficient garbage processing system, ultimately speeding up the aging process of brain cells.
It’s evident that the impact of COVID-19 infection on the brain and nerves is multifaceted and comprehensive. This damage is far-reaching and long-lasting, and very difficult to recover from.
One phenomenon is worth noting. That is, the study mentioned that the incidence of mood disorders and anxiety in COVID-19 patients was transiently increased, suggesting that these symptoms might be caused by some transient triggers. The causes of such mood disorders and anxiety are different from the mechanism of normal neuron cell death and loss due to brain fog or dementia.
Mild COVID-19 Infections Can Also Alter the Brain
A study published in Nature in March found that even a mild COVID-19 infection can alter the brain.
In this study, Oxford University neuroscientists used UK Biobank’s bio- specimens from nearly 800 participants, half of whom were COVID-infected and the other half were uninfected. Ninety-six percent of them weren’t hospitalized, suggesting that most were mildly infected.
These subjects underwent magnetic resonance imaging of the brain before and after infection. The researchers analyzed the structural changes in their brains and found three major ones.
First, COVID-infected participants had a significant reduction in brain volume, commonly known as brain atrophy, suggesting a possible increase in the incidence of dementia. Compared to the control group, the average extra loss of brain volume was 0.2 percent to 2 percent in the COVID-infected patients.
Second, the areas of the brain with reduced volume are mainly the orbitofrontal cortex (associated with decision-making processes), and the gray matter thickness of the parahippocampal gyrus (associated with cognition, emotion, and memory). Here, volume was lost to a greater extent, suggesting an increased risk of brain fog.
Third, the damage to areas associated with the olfactory cortex was also significant.
More importantly, this suggests that the SARS-CoV-2 virus’s damage to the brain isn’t related to the severity of the disease. Structural and functional abnormalities of the brain can occur even in mild cases.
As aforementioned, Omicron infection doesn’t have a high rate of severe disease or mortality, which means that there are a lot of mild cases. However, it can also cause long COVID, the sequelae of the COVID-19 infection, including dementia and neurological diseases, as mentioned in the earlier study.
Of course, studies have reported that the rate of long COVID due to Omicron infection is half of that by Delta. However, because of the large increase of the infected population, the number of long COVID patients due to Omicron isn’t necessarily less than that of the previous variants.
The Brain Has the Ability to Regenerate: Long COVID Can Be Reversed
There’s at least one cause for every disease, and it may be complicated. If the underlying causes can be found and resolved, then the disease may be cured or even reversed.
What’s behind the neurological damage caused by the COVID-19 infection? I have been following the neurological and psychological topic of COVID-19 for a long time, and I have read a lot of research. I also have previous research experience in neurology. According to my understanding and conclusion, although the SARS-CoV-2 virus strikes the human nervous system on seven aspects, the most severe cause lies in the virus’s lethal strike of the neural stem cells.
In other words, the attack of the SARS-CoV-2 virus on neural stem cells leads to the destruction of the mechanism of neural cell regeneration in the brain, which is the crux of the problem.
Even if there appears to be severe damage to the brain, there are still ways to repair it. Scientists have discovered that the human brain has the ability to repair and regenerate itself.
The brain’s regeneration ability was previously thought to be impossible, and this was a conclusion once written in textbooks. Since 1960, scientists have presented convincing evidence that brain nerve cells in adult animals or adult humans can regenerate.
For instance, scientists have found that the hippocampal region produces 600 to 700 new neurons per day. Of course, the brain has a total of 100 billion cells, and these 600 to 700 cells may not seem to be a lot. However, it shows that the brain is capable of regeneration, which is a key mechanism for maintaining brain plasticity and resilience.
And it’s this mechanism that the SARS-CoV-2 virus attacks, and it’s this regenerative power that it inhibits. So to solve the problem of neurological sequelae after the COVID-19 infection, we have to study it from the perspective of regeneration.
The main areas of nerve cell regeneration are the subventricular zone/olfactory bulb (as they are linked together), and parahippocampal gyrus.
The SARS-CoV-2 virus attacks the olfactory bulb and parahippocampal gyrus.
These two areas are like nerve cell manufacturing plants in our body and are the most important locations for nerve cell regeneration. In other words, the SARS- CoV-2 virus attacks the core of the brain—the area responsible for nerve cell regeneration. This is why the sequelae of nerve damage caused by the COVID-19 infection last so long and are so far-reaching.
So how long does the nerve cell regeneration process take?
One would certainly hope that this process is as fast as possible. In fact, nerve cell regeneration isn’t slow. It takes three days for neural stem cells to generate neural progenitor cells, another two weeks to differentiate into naïve nerve cells (i.e., immature neurons), and another four weeks to develop into mature nerve cells. So the entire process usually takes at least six to seven weeks.
Ultra-Simple Aerobic Exercise for Nerve Cell Regeneration
Nowadays, nerve cell regeneration is a popular research topic. Many scientists are using methods such as neural stem cell implantation and neurotrophic factors; however, there are significant limitations in terms of applicability and effects.
I’ve consulted a lot of literature to find methods that are convenient, accessible, and also effective in helping the mind and body. There are, indeed, many more natural methods, and I can introduce them later when I have the opportunity.
Here, I’m presenting to you one of the simplest, cost-free, easy-to-do ways to regenerate neurons that are readily available to everyone. This method is consistent, regular, relaxing, and voluntary aerobic exercise.
It’s generally known that exercise can bring more blood flow to the heart, lungs, and even the brain. However, many people don’t know that regular aerobic exercise can also promote the regeneration of brain nerve cells in adults.
Let’s first take a look at the data from an animal experiment.
In a study at the Salk Institute for Biological Sciences in California, the researchers divided adult mice into two groups. The experimental group had running wheels and other favorable exercise conditions in their cages, while the control group didn’t. It was found that after four weeks of voluntary and relaxing exercise by the adult mice, the regeneration of their hippocampal dentate gyrus nerve cells was significantly increased. The mice in the experimental group had regenerated approximately three to four times more nerve cells than those in the control group.
Moreover, the exercise accelerated the development of their regenerative neurons.
In 2017, some Argentinian neuroscientists published a study in Cell Reports. The experimental design was similar to that of the previous study. This study discovered that after 21 days of exercise, the newly grown neurons of the exercising mice were significantly more mature, with dendrites four times longer and more branched out than those of the sedentary (with no running exercise conditions) mice.
The neurons of sedentary mice in the graph resembled small bean sprouts, while those of exercising mice resembled well-grown bean sprouts.
According to the results of an electrophysiological function test, the granule cells of sedentary mice lacked action potentials or function. The granule cells of the exercising mice were repetitively discharging electricity, indicating that they were transmitting information and communicating with other neurons.
The development of nerve cells is only accelerated after a long period (three weeks), instead of a short period (one week) of exercise. At one week, the nerve cells haven’t yet undergone so many structural and functional changes. So, does effective exercise have to be running?
Not necessarily. Walking, daily grocery shopping, and household chores, which are related to physical activities, are all effective exercises.
How much physical activity should we undertake every day in favor of neuroregeneration? There are two studies that can give us some insights.
The first is a prospective observational cohort study in which 716 older adults without dementia were continuously observed for their daily physical activity over four years.
After four years, 71 subjects developed clinical Alzheimer’s disease, which is a form of dementia, while those with high levels of total daily physical activity had about a 53 percent lower risk of Alzheimer’s disease.
The design of this study was rigorous, and the analysis excluded other confounding factors that might influence the onset of dementia in old age, including age, gender, education, social and cognitive activity, as well as factors such as current level of motor function, depressive symptoms, chronic health conditions, and APOE gene allele status. That is, these confounding factors were balanced in both groups of older adults.
The study concluded that daily physical activity level was an independent predictor of the onset of dementia in the elderly.
In another study, which was more detailed, 299 adults (with a mean age of 78 years) were followed up to examine the association between gray matter volume, physical activity, and cognitive impairment.
In this study, physical activity was calculated as the number of blocks walked in a week, and gray matter volume was an index associated with brain regeneration.
Based on their amount of physical activity, the investigators divided the 299 subjects into four groups from Q1 to Q4 (Q1 group had the lowest activity, and Q4 group had the highest activity). After observing them for 13 years, it was discovered that the gray matter volume in the Q4 group was significantly larger than those of the other three groups with less amount of physical activity. This difference was statistically significant, while there was no difference in the gray matter volumes of the other three groups.
Furthermore, the Q4 group had a twofold lower risk of cognitive impairment than the other groups after 13 years.
So, how much did the Q4 group walk each week?
They walked a cumulative total of 72 blocks per week (around six to nine miles per week).
Therefore, we can tailor the amount of workout and exercise to our own conditions.
So, reflecting on the fact that during the COVID-19 pandemic, lockdowns have been imposed across the globe, and some people couldn’t go out and exercise freely, it wasn’t beneficial to the neuroregeneration of their brain.
The Body Needs an Organic Balance of Movement and Stillness
Some health signals are simple yet easily overlooked. In fact, the human body and mind are closely related.
In addition to the need for nutrients such as glucose and oxygen, the brain’s self- repairing and regenerative functions are facilitated by daily soothing, relaxing, and voluntary exercise.
We have previously mentioned the benefits that sitting in meditation brings to the brain. This isn’t necessarily conflicting with the exercise advice. The human body is one organic equilibrium that requires a balance of movement and stillness. If our movement and stillness can be dynamically balanced well, our brains benefit from such dynamic equilibrium quite a lot.
This is why we have always emphasized that aerobic exercise that makes you feel comfortable is the best. We can all arrange it appropriately according to our life and work schedule.
There’s a saying: “Walking a hundred steps after each meal can help you live to be 99 years old.” Such exercise is not only helpful to our intestines and digestion, but also beneficial to our brain and nerve regeneration. It’s easy, cost-free, and natural. It could potentially help us to prevent premature aging and the neurological/psychological sequelae of COVID. Here, you can see again another example of how one small, healthy habit could make us healthier and even change our lives.
Download a pdf of this article here
…………….
Additional Sources Of Information
• Early Onset Dementia Is Being Caused By The Covid Vaccine (~25X increase) (Steve Kirsch, 08/20/23)
• Psychosis Associated With COVID-19 Vaccination (psychiatrist.com – 02/17/22)
• Can New Onset Psychosis Occur After mRNA Based Covid-19 Vaccine Administration? A Case Report (PubMed Central – 08/08/21)
• Articles on The Epoch Times that mention “COVID-19 vaccines and psychosis”
…………….
Return To Main COVID-19 Resource Page
…………….